Cervical cancer is one of the most common cancers affecting women worldwide, yet it is also one of the most preventable. According to the World Health Organization (WHO), approximately 600,000 women are diagnosed with cervical cancer each year, and over 340,000 lose their lives to it. The encouraging news is that with proper education, regular screening, and an understanding of the key risk factors, women can take meaningful steps to protect their health.
This article provides an in-depth look at what cervical cancer is, how it develops, who is most at risk, and — critically — how certain lifestyle and behavioral patterns can either increase or reduce that risk. We will also explore the connection between sexual behavior patterns and cervical cancer risk, a topic that is backed by decades of medical research and is essential for women to understand.
What Is Cervical Cancer?
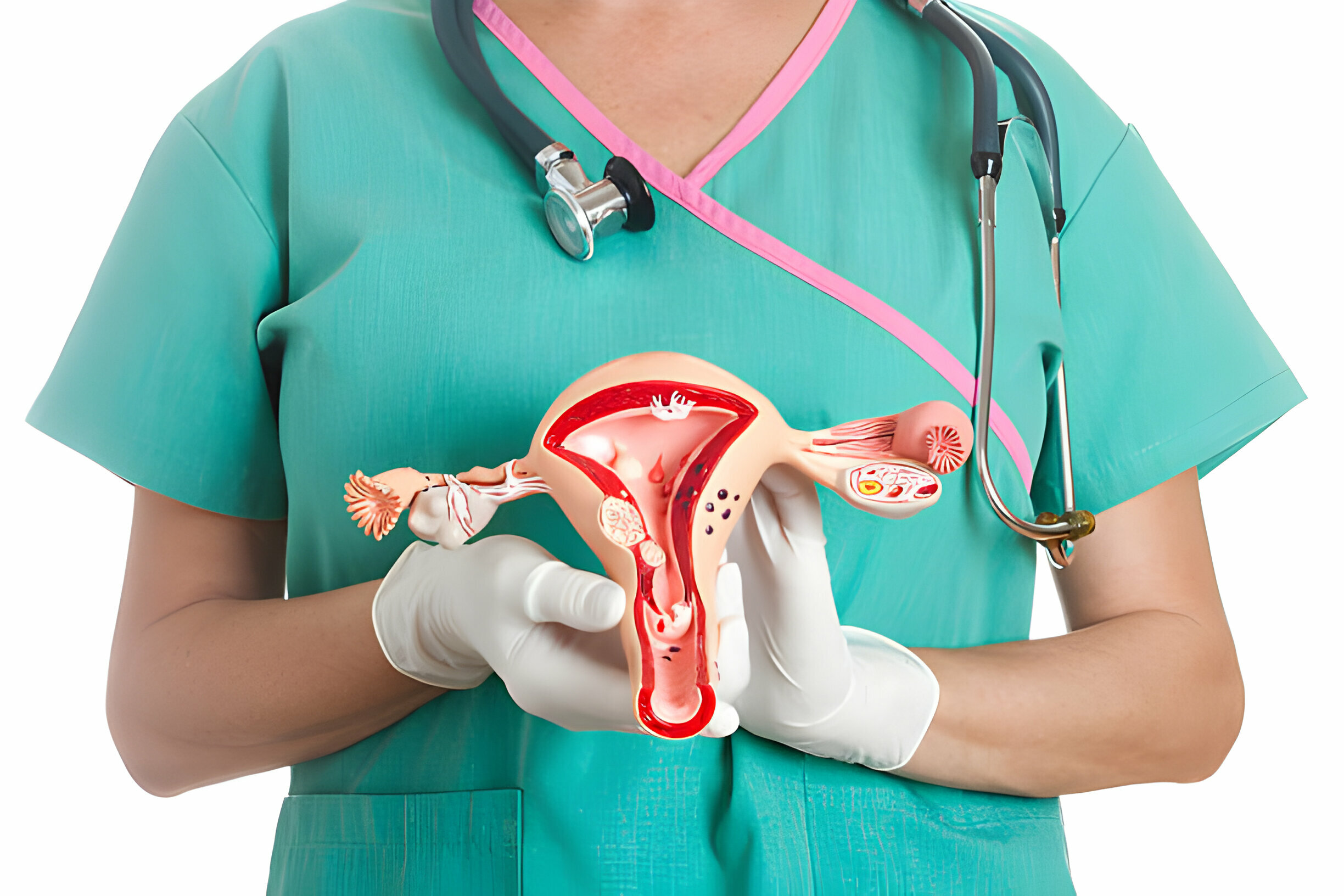
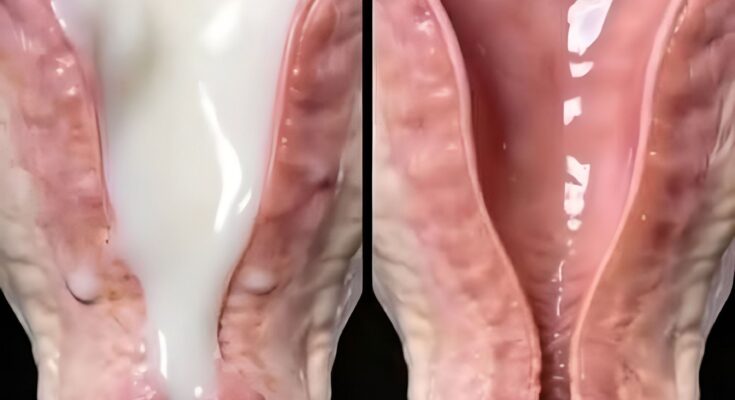
Cervical cancer originates in the cells of the cervix, which is the lower, narrow portion of the uterus that connects to the vagina. Most cervical cancers begin in the transformation zone — the area where the cervix transitions between two types of cells: squamous cells (flat cells lining the ectocervix) and glandular cells (column-shaped cells lining the endocervix).
The two main types of cervical cancer are squamous cell carcinoma, accounting for about 70–90% of all cases, and adenocarcinoma, which develops from the glandular cells. In rare cases, both types may be present simultaneously. Cervical cancer is usually slow-growing, taking years to develop from precancerous lesions into full-blown cancer — which is exactly why early screening is so powerful.
The Root Cause: Human Papillomavirus (HPV)
Virtually all cases of cervical cancer — more than 99% — are linked to persistent infection with high-risk strains of Human Papillomavirus (HPV). HPV is the most common sexually transmitted infection in the world; most sexually active individuals will be exposed to it at some point in their lives. In the majority of cases, the immune system clears the virus naturally within one to two years without causing any harm.
However, when a high-risk HPV strain — particularly HPV-16 or HPV-18 — persists in the body, it can cause changes in cervical cells over time, eventually leading to precancerous conditions and, if untreated, invasive cancer. There are more than 200 types of HPV, of which about 14 are considered high-risk. Understanding how HPV is transmitted is fundamental to understanding cervical cancer risk.
Key Risk Factors for Cervical Cancer
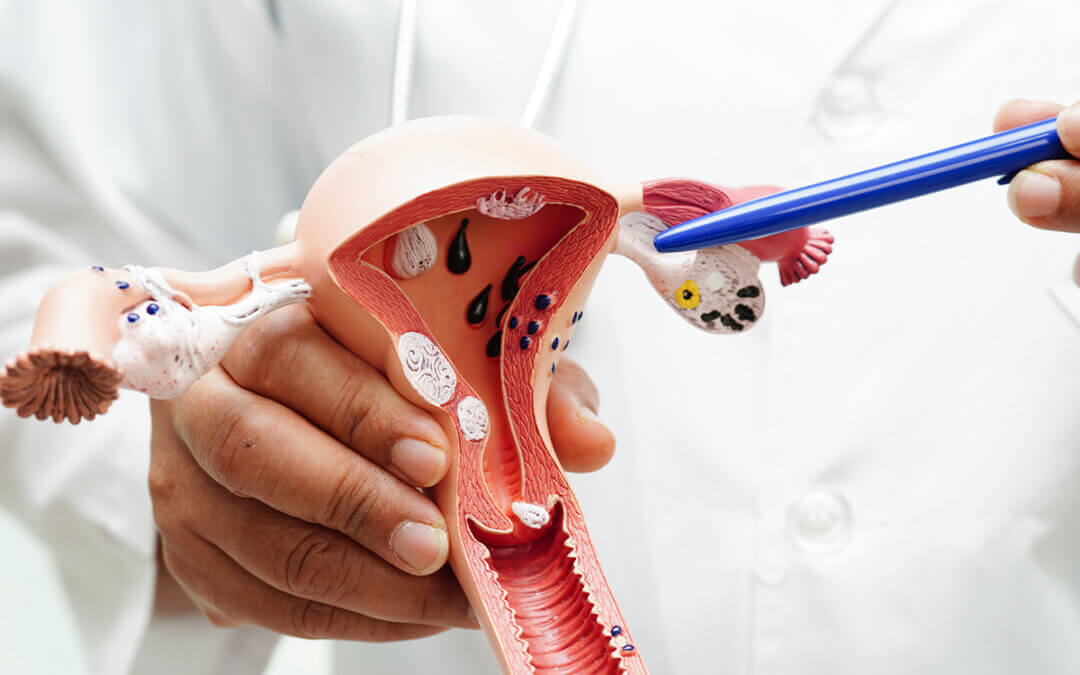
While HPV infection is the primary driver of cervical cancer, not every woman who gets HPV will develop cancer. Several risk factors can increase the likelihood of progression from HPV infection to cervical cancer:
1. Number of Lifetime Sexual Partners
One of the most well-documented risk factors for cervical cancer is having multiple sexual partners over a lifetime. This is not a moral judgment — it is a straightforward matter of epidemiology. Because HPV is primarily transmitted through intimate skin-to-skin contact during sexual activity, a woman who has a higher number of sexual partners has a statistically greater chance of being exposed to one or more high-risk strains of HPV.
Research consistently shows that women with six or more lifetime sexual partners face a significantly elevated risk of HPV infection compared to women with fewer partners. A landmark study published in the Journal of the National Cancer Institute found that the risk of HPV infection — and by extension, cervical cancer — increased incrementally with each additional partner. The reason is simple: each new sexual partner represents a potential new source of viral exposure, including strains the woman may not have previously encountered.
Importantly, it is not only a woman’s own number of partners that matters. If a woman’s partner has had many previous partners, that also increases her risk, since her partner may carry HPV strains acquired from other individuals. This is why open, honest communication between partners about sexual health history — combined with regular screening — is so important.
2. Early Sexual Activity
Beginning sexual activity at a young age is another recognized risk factor. The cervical cells in adolescents and young women are still maturing, which makes them more susceptible to HPV infection. Women who become sexually active before the age of 18 have a higher lifetime risk of HPV exposure, partly due to biological vulnerability and partly due to the longer cumulative period of potential exposure.
3. Weakened Immune System
Women with weakened immune systems are less equipped to clear HPV infections naturally. This includes women living with HIV/AIDS, those who take immunosuppressive medications following organ transplants, or individuals with autoimmune disorders. A compromised immune system allows HPV to persist longer, raising the likelihood of cellular changes that can lead to cancer.
4. Smoking and Tobacco Use
Women who smoke are roughly twice as likely to develop cervical cancer compared to non-smokers. Tobacco byproducts have been detected in the cervical mucus of smokers, where they can damage the DNA of cervical cells. Smoking also suppresses local immune responses in the cervix, making it harder for the body to fight HPV infection effectively.
5. Long-Term Use of Oral Contraceptives
Studies suggest that women who use oral contraceptives for five or more years may have a modestly elevated risk of cervical cancer, particularly among HPV-positive women. The exact mechanism is not fully understood, but hormonal influences on HPV persistence and cervical cell behavior are believed to play a role. Risk appears to decrease after discontinuation.
6. Lack of Regular Screening
Perhaps the most preventable risk factor is simply not getting screened. Many women diagnosed with advanced cervical cancer had never received a Pap smear or HPV test. Regular cervical screening allows healthcare providers to identify precancerous changes early — long before they develop into invasive cancer.
Why Multiple Partners Elevates Risk: The Science Explained
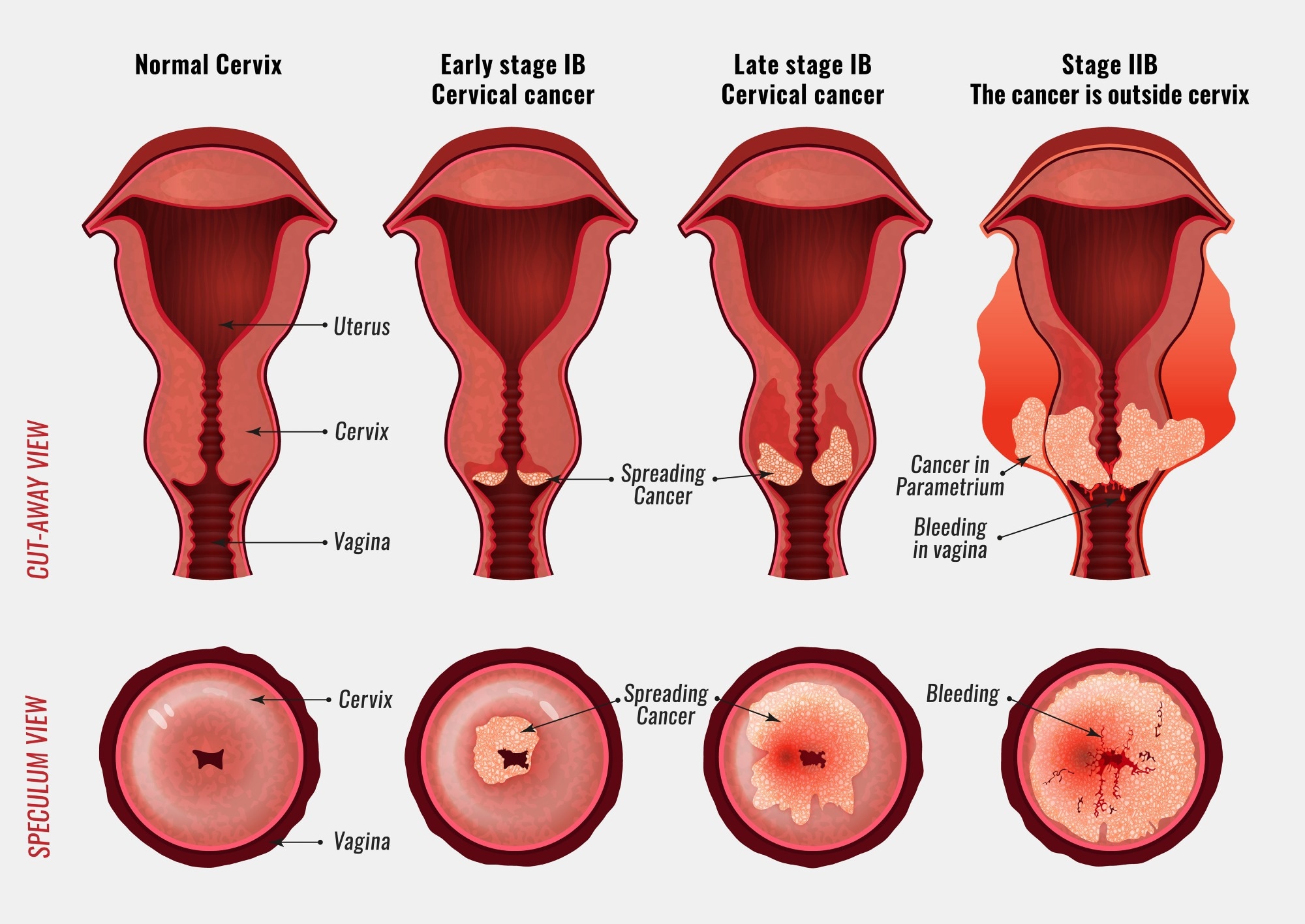
It is worth diving deeper into the relationship between sexual behavior and cervical cancer, because the evidence is both robust and widely misunderstood. Having multiple sexual partners over a lifetime is associated with higher HPV acquisition rates simply because of the mathematics of exposure. Each partner introduces the possibility of carrying and transmitting a different HPV strain — or a high-risk strain the woman has not yet encountered.
A major multinational study by the International Agency for Research on Cancer (IARC) analyzed data from thousands of women across multiple countries and found a clear, consistent dose-response relationship: as the number of sexual partners increased, so did the prevalence of high-risk HPV infection. Women with 10 or more lifetime partners had HPV prevalence rates several times higher than women with one lifetime partner.
The same pattern holds true when considering a partner’s sexual history. If a woman has one partner, but that partner has had many previous relationships, the woman’s risk profile changes accordingly. This is why some researchers describe cervical cancer risk as reflecting a network of sexual contacts, not just direct behavior. HPV can remain dormant for years and can be transmitted to new partners long after the original infection.
To be clear: not every woman with multiple partners will develop cervical cancer, and some women with very few partners can still be affected. Risk factors do not determine destiny — they shift probabilities. The good news is that both vaccination and screening dramatically reduce the consequences of HPV exposure, regardless of a woman’s relationship history.
Symptoms: What Women Should Watch For
Early-stage cervical cancer often causes no symptoms, which is one of the reasons regular screening is so critical. As the disease progresses, women may notice:
- Unusual vaginal discharge, which may be watery, bloody, or have an unpleasant odor
- Vaginal bleeding between menstrual periods, after intercourse, or after menopause
- Pelvic pain or pain during intercourse
- In advanced stages: back pain, leg swelling, difficulty urinating, or loss of bladder/bowel control
Any of these symptoms warrant prompt medical evaluation. Many are caused by conditions other than cancer, but it is always better to be evaluated early.
Prevention: Empowering Women to Reduce Their Risk